Geography is the enemy.
That’s what it all comes down to for a woman who lives in a sparsely populated area if she is dealing with a complicated pregnancy.
High-risk pregnancies require regular monitoring, yet women in rural areas often find it difficult to drive several hours one or more times a week to see a specialist. So they routinely delay, or skip, appointments.
That can have serious consequences. Tennessee has the sixth highest infant mortality rate in the nation, and more than $600 million is spent in the state every year on costs related to poor birth outcomes.
“Getting people in rural areas to see a physician can be a challenge, and when I came out of medical school I thought we could put resources on a tractor-trailer and drive into those communities,” says Dr. David Adair, of Chattanooga’s Regional Obstetric Consultants. “But the expense made that impossible.”

STORC leverages technology to connect women to their doctors.
So in 2012, Dr. Adair implemented the Solutions to Obstetrics in Rural Counties (STORC) program, which uses telemedicine technology to connect pregnant women to physicians who specialize in high-risk pregnancies.
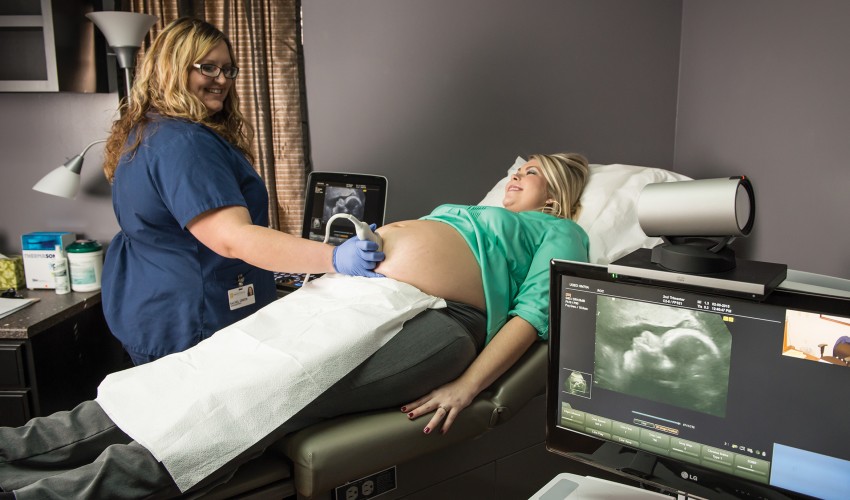
The setup is pretty simple: A camera is connected to a desktop PC, and the woman visits with the high-risk pregnancy specialists at Regional Obstetrical Consultants just as she would if they were in the same room.
 Her local physician provides lab results and other information, and a traveling treatment team is on hand to facilitate the virtual consultation.
Her local physician provides lab results and other information, and a traveling treatment team is on hand to facilitate the virtual consultation.
For local doctors, a lifeline
At Namaste OB-GYN in McMinnville, STORC has been a game changer, says Dr. Dawnmarie Riley. Because her practice deals with a large number of high-risk cases, a STORC telemedicine unit is in her office about three times a week.
“We have trouble with compliance, because patients just find it too difficult to go to Chattanooga, Nashville or Murfreesboro repeatedly,” Dr. Riley says.
And even though some patients may balk at a remote consultation, she quickly overcomes that by pointing out that all services are the same, and seeing the specialists on a screen negates a long, uncomfortable drive.
“They usually decide that the ‘doc in the box’ is OK after that,” she laughs.
Dr. Riley has another good reason to tout the program: Her daughter, McKenzie Jacobs, is a two-time STORC user.
“They stepped in right away and met us at the hospital,” Dr. Riley says of McKenzie’s second hospitalization and delivery. “I was on call when she began having problems, but I needed to be her mother, not her doctor. I can’t say enough about the good work that Dr. Adair’s group and STORC are doing in taking care of some very sick mothers and babies.”

Dr. Dawn Marie Riley’s daughter, McKenzie, used the telemedicine technology during both her pregnancies.
To read more about healthy kids in Tennessee, click here.
Photos by Wolf Hoffman.
The post Special Delivery appeared first on Better Tennessee.